A scalable solution for inflammation research
Olink® Explore
High-throughput biomarker discovery
Learn more
Olink® Target
Targeted biomarker analysis
Learn more
Olink® Flex NEW!
Build your own panel of up to 21 protein biomarkers
Learn more
Olink® PEA
One scalable platform. Endless possibilities.
Learn more
Inflammatory protein biomarkers of human diseases
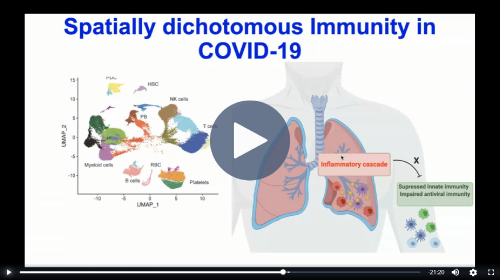
 Cytokine release syndrome in severe COVID-19
Cytokine release syndrome in severe COVID-19
 Neurological diseases and neuroinflammation
Neurological diseases and neuroinflammation
 Inflammatory Bowel Disease (IBD)
Inflammatory Bowel Disease (IBD)
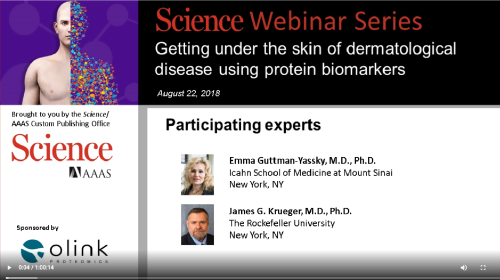
 Dermatological diseases
Dermatological diseases
"We are now experiencing a translational revolution in inflammatory skin diseases"
Professor Emma Guttman discusses why inflammatory protein biomarker analysis is revolutionising her dermatology research and how Olink technology has been instrumental in her work.
Olink has an outstanding track record in inflammatory protein biomarker research.
Deeper understanding of inflammatory mechanisms in disease will improve diagnosis
Olink’s inflammatory protein assays have been widely used by our customers. In 1013 peer-reviewed publications citing Olink up to October 2022, almost half of these studies (47%) used our specialty panels for inflammation-related proteins.
Olink inflammation assays have been used in studies across a wide range of disease areas such as COVID-19 , neuroinflammation, IBD and dermatological disease. To get a flavor of some of the highlights you can read more below.
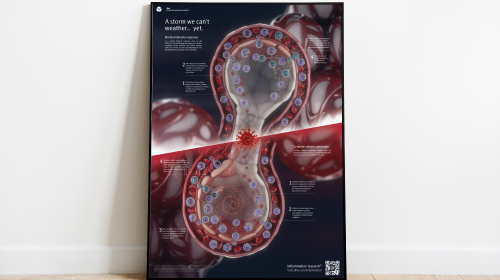
A storm we can't weather... yet.
The COVID-19 pandemic emphasized the disastrous potential of inflammatory molecules, where “cytokine release syndrome” resulting from excessive immune responses to the virus were responsible for severe/fatal outcomes in some patients. Olink has an outstanding track record in COVID-19 related research.
Add color and flair to your lab with our free poster explaining cytokine storm syndrome in the context of COVID-19. Based on research comparing five clinical studies using Olink data to understand COVID-19 severity, the poster demonstrates this key contributor to severe disease in vivid detail.